Laboratory of Brain Atlas and Brain-Inspired Intelligence Reveals Thalamic Electrophysiological Features in Patients with Disorders of Consciousness
Font:【B】 【M】 【S】
Recently, a collaborative team from He Jianghong's group at Beijing Tiantan Hospital, Capital Medical University; Yu Shan's team at the Laboratory of Brain Atlas and Brain-Inspired Intelligence, Institute of Automation, Chinese Academy of Sciences; Zhang Wangming's group at Southern Medical University; and Steven Laureys, former president of the International Society for the Science of Consciousness, published a study titled Electrophysiological characteristics of CM-pf in diagnosis and outcome of patients with disorders of consciousness in the leading journal Brain Stimulation. The study collected and analyzed the world's largest dataset of thalamic activity recordings in patients with disorders of consciousness (DoC), reporting a series of thalamic features closely related to patients’ condition severity and recovery prognosis.
Disorders of consciousness (commonly known as "vegetative state") refer to severe brain injury caused by trauma, stroke, or hypoxia, leading to prolonged impairment of awareness or wakefulness. Patients can remain unconscious for months, years, or even decades, with unpredictable chances and timing of recovery, imposing heavy burdens on families and society. Understanding the pathological mechanisms of DoC, especially the neural basis of consciousness impairment and recovery, is key to developing effective treatments.
To address this critical clinical and basic science question, the study collected and analyzed thalamic activity recordings from 23 patients with DoC. Overcoming challenges such as low activity levels, complex etiology, and limited sample sizes, the team identified a series of important electrophysiological features significantly associated with the severity of consciousness impairment and recovery levels. These findings provide crucial insights for understanding DoC mechanisms and optimizing clinical treatment strategies.
In recent years, neuromodulation therapies such as deep brain stimulation (DBS) have attracted wide attention for treating conditions like Parkinson’s disease, epilepsy, and depression. Since 2007, DBS targeting the central thalamus has been considered potentially beneficial for arousal in DoC patients. However, the relationship between thalamic activity and DoC severity or the likelihood of recovery remained unclear, limiting the effectiveness of DBS in treating DoC. Therefore, detailed study of thalamic electrophysiological features in DoC patients is important both for understanding the pathophysiology of consciousness impairment and recovery, and for optimizing DBS electrode targeting and treatment strategies.
The study first validated the therapeutic effect of central thalamic DBS. The authors collected electrophysiological signals from the central medial-parafascicular (CM-pf) nuclei of the thalamus during DBS implantation surgery in DoC patients, all of whom subsequently underwent one year of DBS treatment. Clinical results showed that 47.8% of patients improved their level of consciousness after DBS, with eight patients demonstrating good recovery characterized by repeatable command-following, functional object use, or communication ability.
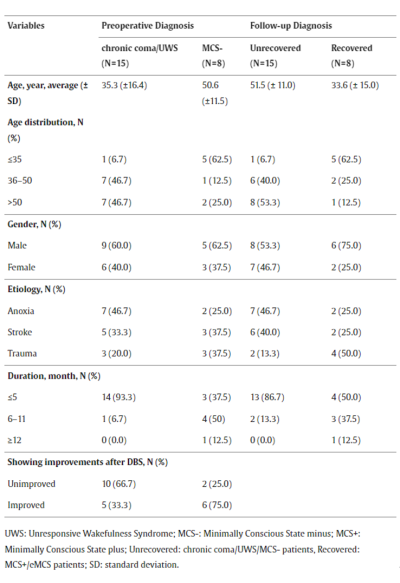
Table 1. Patient information statistics
Further, the study analyzed CM-pf thalamic electrophysiological signals to investigate their relationships with pre-treatment DoC severity and post-treatment recovery outcomes. Given the challenges of sparse single-neuron firing and low signal-to-noise ratio in DoC patients, the authors innovatively used multi-unit activity (MUA) to measure neuronal activity, enabling the extraction of synchronized local population activity from signals that otherwise appear as background noise. Specifically, the authors analyzed five categories of electrophysiological features in the CM-pf nuclei, including neuron firing characteristics, MUA properties, signal stability, MUA–spike synchronization (syncMUA), and background noise levels. The results showed that patients with milder pre-treatment impairment (MCS-) had stronger syncMUA gamma-band synchronization and higher normalized MUA power in the alpha band. Moreover, patients with better post-treatment recovery exhibited stronger metrics across several indicators: firing rate, high-gamma MUA power, alpha-band normalized power, and especially theta-band stability. Among these, theta-band MUA stability was most strongly correlated with recovery outcomes—patients with more stable theta-band MUA showed better consciousness recovery after treatment.、
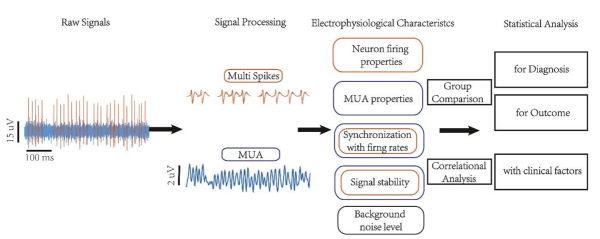
Figure 1. Data analysis pipeline
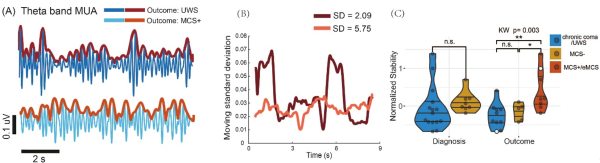
Figure 2. Stability of theta-band MUA
Finally, the authors analyzed the relationship between CM-pf electrophysiological features and major clinical factors. Over the past two decades, numerous studies have highlighted the importance of clinical factors such as etiology, age, and disease duration in understanding consciousness impairment and recovery. However, the electrophysiological correlates of these clinical factors remained unclear. Given the central thalamus's critical role in DoC and recovery, the authors explored these relationships as well. They found that etiology (stroke vs. hypoxia) showed strong associations with CM-pf electrophysiological features. For example, hypoxic patients had significantly lower firing rates (p < 0.001, r = -0.68). Considering earlier findings that patients with lower firing rates had worse prognoses, this explains the clinical observation that hypoxic brain injury often leads to poorer recovery. In contrast, stroke patients showed relatively higher CM-pf metrics, as did patients with traumatic brain injury. Although clinical observations suggested younger patients tend to recover better, the study did not find significant correlations between age and CM-pf features.
In summary, this study conducted a comprehensive analysis of CM-pf thalamic electrophysiological features in DoC patients, revealing that these features are critical for understanding the pathophysiological mechanisms of DoC, predicting recovery, and explaining the influence of clinical factors. These findings deepen our understanding of the neural mechanisms underlying DoC and recovery and provide important clues for optimizing future treatment strategies.
He Jianghong from Beijing Tiantan Hospital, Capital Medical University, and Zhang Haoran, a PhD student at the Institute of Automation, Chinese Academy of Sciences, are co–first authors of the paper. Zhang Wangming from Zhujiang Hospital, Southern Medical University, and Yu Shan from the Institute of Automation are co–corresponding authors. The study was supported by the National Natural Science Foundation of China and the CAS International Cooperation Program.
Paper link:
https://doi.org/10.1016/j.brs.2023.09.021
Copyright Institute of Automation Chinese Academy of Sciences All Rights Reserved
Address: 95 Zhongguancun East Road, 100190, BEIJING, CHINA
Email:brain-ai@ia.ac.cn